Drake LeBrun
Thomas J. Watson Fellow 2012Project
Surgical Disparities in the Developing World
Peru, Bolivia, Bangladesh, Thailand, Malaysia, Switzerland, Tanzania
Follow Drake's journey

As a child, I dreamed of becoming a surgeon. I was going to work hard through high school and college, get into medical school, become a surgeon and save lives, using cutting-edge techniques and the latest medical technology. My Watson year would alter that trajectory forever.
In my first days in Peru I had no idea what I was doing. I’d arranged to shadow surgeons in a hospital in Lima, but that wasn’t going to start for a few weeks, and so I spent my time wandering the city, improving my elementary Spanish, and seeking out Peruvian food. I was lonely, but life seemed fairly easy.
Lima, Peru
Flash forward three and half months. Everything’s different; Lima already seems like a lifetime ago. I’m sitting behind a tiny hospital in the town of Pucallpa, deep in the Peruvian Amazon, working with a team of American orthopedic surgeons who’d flown in for a week-long surgery clinic. I’d been helping out in the sweltering, mosquito-plagued operating room for 15 hours a day, wiping the surgeon’s faces as they operated so they wouldn’t sweat into an open body cavity.
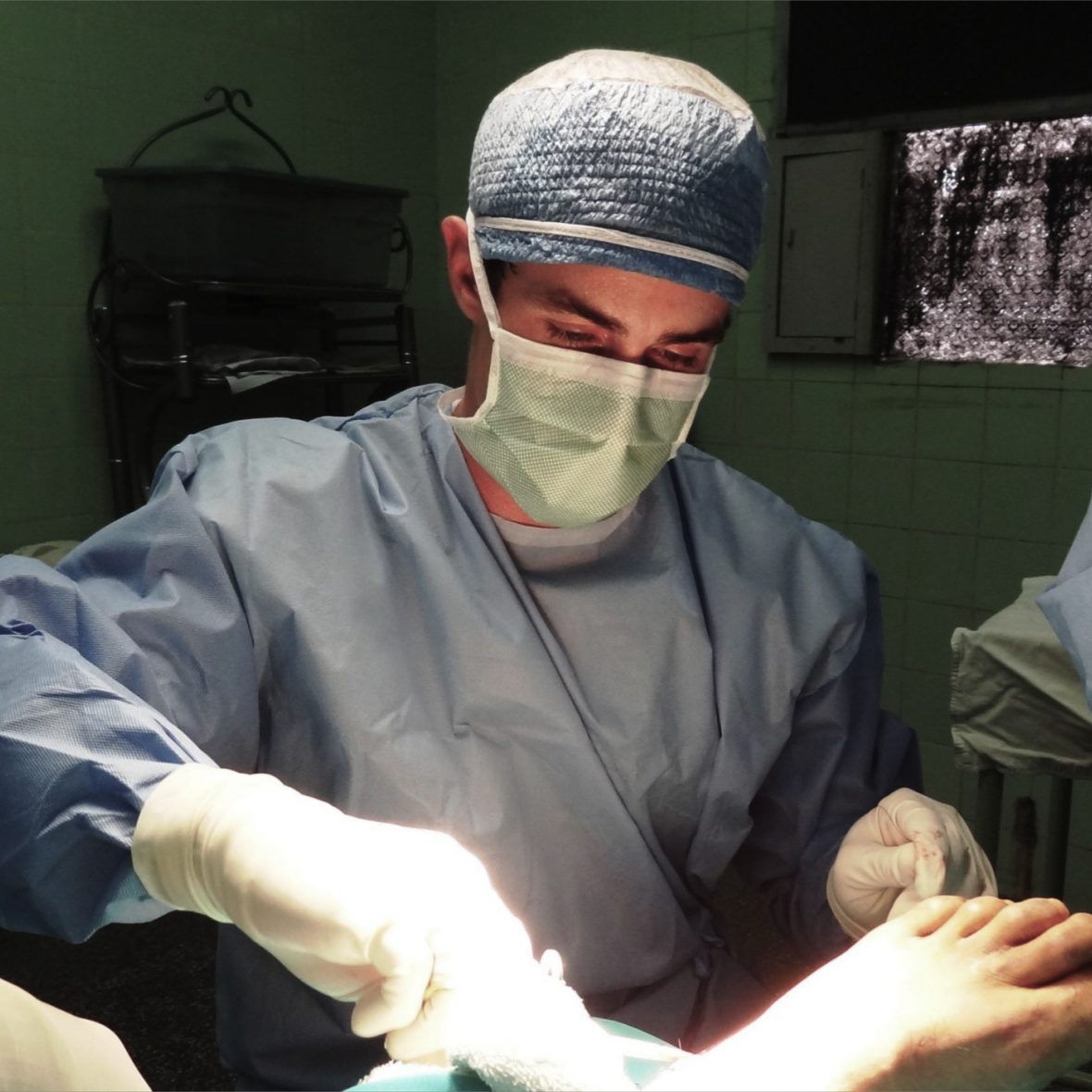
In the operating room
Pucallpa, Peru
Once, when a patient woke from anesthesia during a procedure, I had to calm him down since I was the only person in the room who spoke Spanish. During a break, one of the doctors took me aside and said, “Do you know how to suture?”. “No,” I replied. “Well,” he said, “get a banana.” I found one and watched as he peeled it and then began to stitch it closed. Then he handed it to me and told me to finish the job. A few days later, he watched over me as I sewed up the leg of a patient who’d arrived with a broken femur. This was way beyond what I’d expected from my Watson year, and I wasn’t even halfway done.

Bolivia
Bangladesh took me by surprise in another way. I had no idea what to expect when I boarded the plane to Dhaka—literally, since the project I’d tried to organize there had fallen through. I’d taken a deep breath and decided to go anyway, with a single contact and an idea based on the project I’d just done in Bolivia, where I’d tried to assess the state of the country’s surgical resources. But what I really wasn’t prepared for was that when I arrived, the family in whose care I landed would welcome me like a long-lost relative. The father in the family, a banker, put me in touch with friends and relatives across the country, and even facilitated contacts for me in opposing political parties. The next few weeks were a whirlwind of traveling, small towns and hospital chiefs, but what stayed with me was the kindness my hosts extended to a strange foreigner while asking nothing in return.
Bangladesh
Having spent the previous nine months in developing countries, I experienced a powerful ‘reverse’ culture shock in Geneva, the headquarters of the World Health Organization. I’d come from Malaysia, where I could pay 50 cents for dinner on the street, to one of the world’s most expensive places, surrounded by snowy alps and a glacial lake so clean I could drink from it. Most welcome, however, was that for the first time on my year I found myself among people who shared my growing passion for global health and medicine, and it was wonderful to be able to talk about the urgent need I’d seen for more surgical resources in the developing world. To my surprise, this wasn’t an aspect of global health that had received a great deal of attention; the WHO has often focused on the treatment and prevention of disease, but not as much on trauma—and I started to see a space in the world of global medicine that I could occupy.

Switzerland
Geneva also gave me time to reflect on my desire to become a surgeon. Surgeons don’t tend to get involved in global health issues, partly because there’s always a need for them at home. I wonder, though, if surgeons also tend to be attracted to the OR’s unambiguous world of acute problems and quick fixes: let’s set this bone. Let’s deliver this baby. Let’s save this life. In the world of global health, however, there are seldom quick fixes. My Watson year had convinced me that lack of access to surgery is a global problem, one that I could help to solve. My childhood dream was intact, but my idea of the kind of surgeon I wanted to be was changing.
My Watson year ended in the tiny town of Ifakara, Tanzania—one dirt road, one hospital. Though I was the only foreigner in town, it felt like home after a few short weeks. The hospital staff became my family; the Njema Guesthouse, my house; the little restaurant on a street corner, my kitchen. In the St. Francis Referral Hospital (370 beds), I walked the wards, talked with doctors, nurses, and patients, and came face to face with one of rural Tanzania’s greatest healthcare challenges: untreated trauma. People came in with terrible injuries they’d suffered from vehicle accidents and—surprisingly often—falling from trees. You’d see these kinds of injuries in a US trauma unit too, but with a crucial difference: the injuries here had often happened weeks ago. Wounds and broken bones had become dangerously infected, often posing more of a hazard to the patients’ lives than the injuries themselves. That’s what happens without access to the kind of immediate care I took for granted back home, the speeding ambulance and the wailing siren. The surgeons at the hospital were heroic people, with little in the way of personal lives; they were dedicated to their patients and their community, and they worked 12-hour days and were on call almost all the time. Once again, I felt humbled by the people around me, and though the prospect of going home to my family, my girlfriend, and a mosquito-free bedroom was an appealing one, I had to face a strange truth in my last days at Ifakara: I had never been happier in my life.

Tanzania
Where they are today
Orthopedist, Hospital for Special Surgery | New York, New York
Our Programs
Our Fellows
Through one-of-a-kind programs we encourage students to create personal pathways, then support their journeys.